
Pictured are three Ugandan research assistants learning how to use the device. Benard Tumwesigye is using the device on Anna Nakirabira while Medius Kyakuhaire looks on.
Published September 19, 2022, last updated on September 29, 2022 under Around DGHI
In Uganda, limited access to expensive CT scanning equipment can mean patients with brain injuries often face long waits before they can be examined, delays when issues such as internal bleeding could become critical. But Duke brain scientists are hoping a pocket-sized scanner could offer a much more accessible and affordable option.
The handheld device, developed by InfraScan, has been approved for use on patients in the United States and elsewhere to detect intracranial bleeding. Researchers with Duke Global Neurosurgery and Neurology (DGNN) led a study of the device’s use among 500 patients at Duke University Hospital, finding it detected bleeding in 100% of patients needing surgery, according to a press release in August.
But the device’s portability and low cost could make it a valuable tool in low-resource settings, says Tony Fuller, M.D., DGNN’s associate director and an affiliate of the Duke Global Health Institute.
“In places like Uganda, a patient could be waiting hours or days before getting scanned,” says Fuller. “That gives your injury more time to get worse. So what can you do about this? How can you look into someone’s head without a CT Scan?”
Following the Duke Hospital study, Fuller worked with colleagues at Mbarara Regional Referral Hospital In Uganda to train three surgical assistants to use the device. It was tested on more than 650 patients aged 12 and older between November 2020 and July 2022. Results are still being analyzed, but they appear promising.
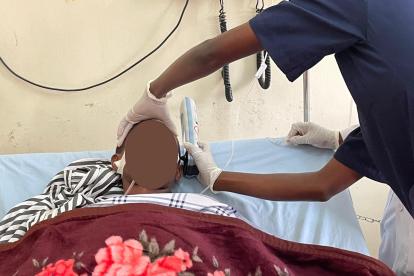
Anna Nakirabira, a research assistant in...
The device uses near-infrared technology to detect the presence and location of brain bleeds, says Josephine Najjuma, a program coordinator at the Mbarara hospital and an assistant lecturer at Mbarara University of Science and Technology.
“It will even estimate how big the bleed is on screen,” Najjuma says. “With the InfraScanner, it can take less than two minutes to find a brain bleed.”
MRRH treats patients from 13 districts and its neighboring countries – Rwanda, Burindi and the Democratic Republic of the Congo. It has only one CT scanner and a second at a private hospital in the same town, which can cost a hospital millions of dollars to buy and thousands to repair. Patients also bear the cost of CT Scans. Without insurance, out-of-pocket expenses can be more than twice a patient’s monthly salary, Fuller notes. The InfraScan device costs from $10,000 to 15,000, he adds.
“For Uganda, this device is cost effective for reasons such as its affordability. It is small and portable and can fit in a doctor’s coat pocket,” Fuller says. “It’s rechargeable and can be used on thousands of patients. It’s easy to repair.”
David Kitya, head of neurosurgery at MRRH and a professor at Mbarara University, says he has seen more trauma patients from traffic accidents in the past decade. The increased use of motorcycles, minimal safety equipment, poor road infrastructure and enforcement of traffic laws has made traumatic injuries a growing global health challenge in Uganda and other low- and middle-income countries.
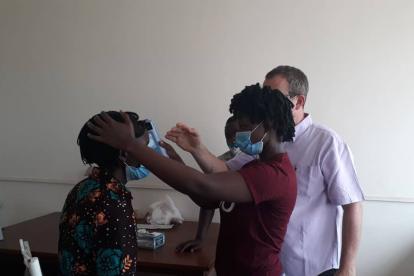
Ugandan research assistants Medius...
“In Uganda, we are worse than our neighbors with traffic injuries,” Kitya says. “There’s a need for us to be able to better care for patients. The diagnosis can be difficult with no [CT] scanners.”
Kitya says integrating the device into continual care can mean shorter wait times and better health outcomes: Fewer patients dying or becoming permanently disabled from undetected brain bleeds.
“You need these types of care in communities so the injured are cared for and people can remain efficient,” he says.
The next phase of the study in Uganda will focus on integrating the InfraScanner into clinical care and researching how it improves patient outcomes. The device’s portability may also make it feasible for use in the field, which is important given Uganda’s rural landscape and lack of access to transportation.
“[Resources] that are portable make it easier to get care to people, and the community doesn’t have to come to you” Fuller says. “It can address most, but not all, equity issues such as reach, access and travel. We [DGNN] are always looking for partnerships because it’s impossible to improve healthcare without collaboration.”


